Assured vs incentX
Side-by-side comparison to help you choose the right tool.
Assured
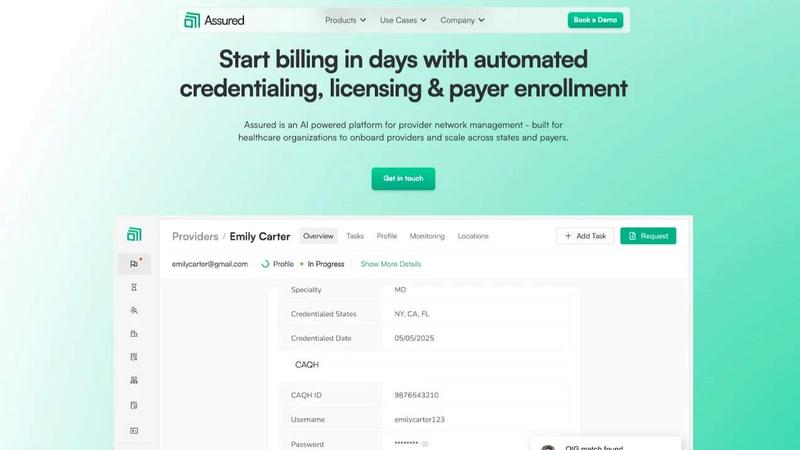
Assured automates provider credentialing and enrollment, enabling healthcare organizations to start billing in days instead of months.
Last updated: April 13, 2026
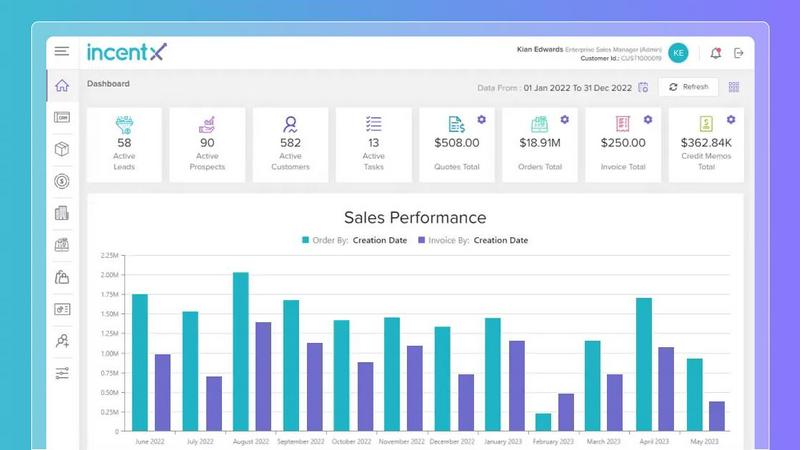
incentX automates incentive compensation with precise, transaction-level accuracy for seamless, error-free payouts.
Last updated: February 28, 2026
Visual Comparison
Assured
incentX
Feature Comparison
Assured
Automated Credentialing
Assured offers end-to-end credentialing that transforms the onboarding process from weeks to days. By automatically verifying provider credentials in real-time across hundreds of primary sources, Assured eliminates the cumbersome documentation and verification tasks that typically delay onboarding, ensuring providers can start seeing patients without unnecessary wait times.
Streamlined Licensing
The platform simplifies the complex landscape of multi-state licensing and renewals, automating the tracking of expiration dates and handling applications across all 50 states. This feature alleviates the administrative burden associated with maintaining compliance, enabling healthcare organizations to scale efficiently while minimizing the risk of administrative chaos.
Efficient Payer Enrollment
Assured accelerates the payer enrollment process, allowing organizations to achieve in-network status 30% faster. By automating submissions and providing real-time tracking of enrollments and follow-ups, Assured ensures that missed deadlines and payer-specific requirements do not hinder timely access to patient care.
Comprehensive Network Management
With Assured’s centralized network management, healthcare organizations can monitor provider data in real-time. This feature aggregates verifications from over 2,000 sources, providing a complete and up-to-date view of provider compliance and status, thus eliminating surprises during audits and enhancing operational transparency.
incentX
Comprehensive Incentive Program Management
incentX offers a unified platform for managing all types of incentive programs, allowing users to run every incentive from the same transaction-level data. This eliminates the need for spreadsheets and disconnected tools, ensuring that every payout is accurate and based on real performance metrics.
Transaction-Level Forecasting
The platform provides unmatched accuracy in predicting payouts by tying commissions directly to fulfilled transactions. This feature helps eliminate commission overpayments and allows organizations to forecast costs by product, team, and region based on actual margin and fulfillment data.
Automated Incentive Calculations
incentX automates incentive calculations, improving accuracy and reducing manual errors. Users can employ transaction-level filters to generate reports by product, region, margin, or representative, offering all stakeholders a transparent view of how each payout is derived.
Real-Time Incentive Visibility
With incentX, organizations can monitor incentives as they occur, making informed decisions based on up-to-the-minute data. This feature enhances sales alignment and allows teams to react swiftly to changes in performance, ensuring that compensation strategies remain effective.
Use Cases
Assured
Rapid Provider Onboarding
Healthcare organizations can leverage Assured to expedite the onboarding of new providers, reducing the time from application to patient interaction significantly. This is particularly beneficial for organizations expanding their provider networks across multiple states, ensuring that specialists can start delivering care without extensive delays.
Multi-State Expansion
For healthcare providers looking to expand their services into new regions, Assured simplifies the licensing and credentialing processes across multiple states. This allows organizations to scale their operations quickly and efficiently, ensuring they meet all regulatory requirements while maintaining high standards of care.
Improved Revenue Cycle Management
By automating credentialing and payer enrollment, Assured helps healthcare organizations minimize revenue loss due to administrative delays. This ensures that providers can begin billing for services sooner, thus improving cash flow and overall revenue cycle management.
Enhanced Compliance Monitoring
Assured enables healthcare organizations to maintain compliance with state and payer regulations through real-time data monitoring. By continuously verifying provider credentials and tracking licensing statuses, organizations can ensure they meet all necessary requirements and avoid potential penalties.
incentX
Sales Compensation Management
incentX enables sales teams to automate payouts using actual ERP transactions, aligning their goals with real revenue, margin, and fulfillment data. This leads to more accurate payouts and fosters trust among sales representatives.
Rebate Program Optimization
Companies can streamline their rebate programs using incentX by leveraging real-time order and claim data. This eliminates the need for shadow accounting and helps maximize the return on investment from rebate initiatives.
Royalty Calculations
With incentX, organizations can calculate royalties based on actual sales data instead of estimates, ensuring that royalty payments are accurate and compliant with audit requirements. This helps protect intellectual property and revenue streams.
Vendor Chargeback Management
The platform allows businesses to match every vendor deduction to actual transactions and returns, offering complete invoice-level visibility. This minimizes disputes with vendors and ensures that all chargebacks are justified and transparent.
Overview
About Assured
Assured is an innovative, AI-powered provider network management platform designed specifically for healthcare organizations aiming to streamline their operations and enhance their revenue generation capabilities. By automating critical administrative tasks such as credentialing, licensing, payer enrollment, and ongoing network monitoring, Assured eliminates the inefficiencies associated with manual processes. Targeted at provider groups, health systems, payers, and digital health companies, it addresses the pressing issues of disconnected data and the slow, error-prone nature of traditional workflows. Assured's key value proposition lies in its ability to dramatically increase speed and accuracy—credentialing providers in as little as 48 hours instead of the usual 60+ days, achieving a remarkable 95% first-pass approval rate for payer enrollments, and identifying sanctions 22 days earlier than conventional methods. As an NCQA-certified Credentials Verification Organization (CVO), Assured seamlessly verifies credentials from over 2,000 primary sources, auto-generates necessary applications, and submits them directly to payer portals, resulting in quicker provider onboarding, accelerated revenue flow, and robust real-time data monitoring—all managed from a single, integrated platform.
About incentX
incentX is a cutting-edge incentive automation platform that transforms how enterprises manage diverse incentive programs, including sales commissions, partner rebates, royalties, trade promotions, and vendor chargebacks. Designed specifically for revenue, finance, and operations teams, incentX addresses the common challenges associated with manual and spreadsheet-driven processes, which often lead to inaccuracies, delays, and disputes. By serving as a single source of truth, incentX leverages direct integration with crucial business systems such as CRM and ERP to ensure that every incentive calculation is based on real, fulfilled transactions rather than unreliable forecasts. This capability allows organizations to achieve real-time visibility into their incentive structures, ensuring accurate and timely payouts while providing audit-ready data. With incentX, businesses can create impactful incentive plans that foster measurable and profitable growth, enhancing their forecasting abilities and financial predictability without heavily relying on IT resources.
Frequently Asked Questions
Assured FAQ
How does Assured reduce provider onboarding time and administrative costs?
Traditional credentialing processes can take over 60 days, burdened by manual and sequential verifications. Assured dramatically cuts this time to just 48 hours by processing applications in parallel and integrating with over 2,000 primary sources. This efficiency translates to annual savings of $4,200 to $5,800 per provider for organizations.
What makes Assured more reliable than traditional methods?
Assured employs advanced AI algorithms to automate complex verification processes, ensuring accuracy and speed. Unlike traditional methods that rely heavily on manual input and are prone to human error, Assured’s automated system provides a higher level of reliability, achieving first-pass approval rates of 95% for payer enrollments.
Can Assured integrate with existing systems?
Yes, Assured is designed to seamlessly connect with various healthcare systems such as Applicant Tracking Systems (ATS), Electronic Medical Records (EMR), and Salesforce using plug-and-play APIs. This integration allows organizations to maintain their existing workflows while enhancing operational efficiency.
What kind of support does Assured provide?
Assured is committed to offering the fastest support in the industry, with a response time of under 24 hours. This ensures that organizations can receive timely assistance whenever they encounter challenges, further enhancing their operational efficiency and peace of mind.
incentX FAQ
What types of incentive programs can incentX manage?
incentX can manage a wide variety of incentive programs, including sales commissions, partner rebates, royalties, trade promotions, and vendor chargebacks, all from a unified platform.
How does incentX improve forecasting accuracy?
By tying commission payouts directly to fulfilled transactions rather than estimates, incentX provides organizations with a more precise method for forecasting costs and payouts, significantly reducing the risk of overpayments.
Can incentX integrate with existing business systems?
Yes, incentX is designed to integrate seamlessly with critical business systems such as CRM and ERP, ensuring that incentive calculations are rooted in actual transactional data.
Is there a support system in place for users of incentX?
Absolutely. incentX offers robust support to its users, including resources for training and customer service to ensure that organizations can fully leverage the platform's capabilities for their incentive management needs.
Alternatives
Assured Alternatives
Assured is an AI-powered provider network management platform that streamlines the complex processes of credentialing, licensing, payer enrollment, and ongoing network monitoring for healthcare organizations. By automating these tasks, Assured enables healthcare companies to start billing in a fraction of the time it would typically take, enhancing operational efficiency and revenue generation. Users often seek alternatives to Assured due to various factors such as pricing differences, specific feature sets, or unique platform requirements that cater to their organizational needs. When exploring alternatives, it is essential to consider the automation capabilities, integration with existing systems, user experience, and the level of customer support offered, as these factors can significantly impact the overall effectiveness of the solution in improving provider onboarding and administrative workflows.
incentX Alternatives
IncentX is a robust incentive automation platform that streamlines the management of various incentive programs, such as sales commissions and partner rebates, through precise, transaction-level accuracy. By serving as a comprehensive solution, it addresses the common challenges faced by finance, revenue, and operations teams burdened by traditional manual processes. Users often seek alternatives to incentX for various reasons, including pricing models, feature sets, or specific platform integrations that better align with their operational needs. When exploring alternatives, it's essential to consider the automation capabilities, the breadth of incentive types supported, ease of integration with existing systems, and the overall user experience. As businesses evolve, the demand for flexible and scalable incentive management solutions grows, prompting users to explore other options. It's crucial to evaluate potential alternatives based on their ability to provide real-time visibility, minimize errors, and ensure compliance with audit standards. A thorough understanding of the specific requirements of your organization will guide you in selecting an alternative that not only meets your current needs but also supports future growth.
